
Brewer, Lorie M. Harper, in, 2018 IntroductionPrune-belly syndrome (PBS), also known as Eagle-Barrett syndrome, is a triad of anomalies composed of abdominal wall flaccidity, urologic abnormalities, and bilateral cryptorchidism. 1–4 The typical urologic findings are distended bladder, hydronephrosis, and renal dysplasia. A patent urachus is a common finding. In some infants, urinary obstruction may lead to oligohydramnios or anhydramnios with a resulting Potter sequence (pulmonary hypoplasia, dysmorphic facies). Concomitant cardiac, orthopedic, and gastrointestinal anomalies are frequent and are reported in approximately 75% of PBS cases. Caldamone, John R.
Woodard, in, 2010Prune-belly syndrome (PBS) is a syndrome with a broad spectrum of severity. It is a constellation of anomalies. The three major aspects are abdominal musculature deficiency, bilateral intra-abdominal testes, and an anomalous urinary tract. The urinary tract is characterized by variable degrees of hydronephrosis, renal dysplasia, dilated tortuous ureters, an enlarged bladder, and a dilated prostatic urethra.
Associated anomalies involving the respiratory tract, gastrointestinal tract, cardiac system, and musculoskeletal systems also occur. There is a broad spectrum of severity of the syndrome, with some children who do not survive the newborn period and others who are minimally affected.
The single most important determinant of survival is usually the severity of the urinary tract anomaly, and in particular, the degree of renal dysplasia. DeMarco MD, in, 2010 INCIDENCEThe incidence of prune-belly syndrome is estimated to be 1 in 30,000 to 1 in 50,000 live births. 8,9 The current incidence may be less, as the Malformations Surveillance Program at Brigham and Women’s Hospital led to elective termination of 31% of children diagnosed prenatally with prune-belly syndrome from 1974 to 1994. 10 Children with incomplete forms of the condition may present with typical abdominal wall changes but no urologic or testicular manifestations.
Also, children may present with classic bladder and ureteral features with little to no involvement of the abdominal musculature. 11,12 The female patient with characteristic abdominal wall and urologic findings is also considered to have an incomplete form of the condition and appears to make up less than 5% of reported cases. From bottom to top, the most common urinary tract anomalies are as follows: ▪The bladder neck is patulous. ▪The bladder is capacious.
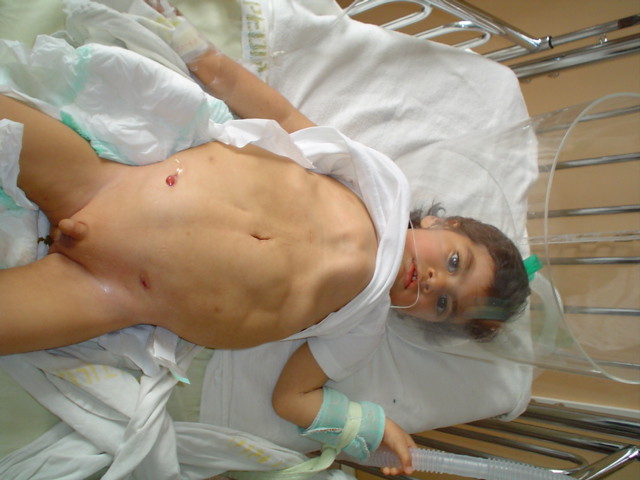
Prune belly syndrome is a birth defect affecting the abdominal muscles, genital organs and urinary tract of the infant. The muscles of the abdomen are poorly developed and the skin covering them.
The bladder wall may be thickened, but the internal contour of the bladder is smooth, without trabeculations or diverticuli. Often the bladder communicates with a patent urachus. ▪Ureteral abnormalities commonly consist of irregular dilations and narrowings, usually most dramatic in the lower ureteral segments. ▪The kidneys are often small, with or without dilation of the collecting system. It is important to note that the anatomic abnormalities of the urinary tract in patients with prune-belly syndrome may be caused by primary, intrinsic, and diffuse defects of embryologic development of the structures involved, which are different from the discrete lesions of obstruction or reflux that may occur in the urinary tract of otherwise normal newborns. However, the abnormalities may appear similar to those that occur in prune-belly syndrome.
For example, the large, thick-walled bladder of patients with prune-belly syndrome may occur in the absence of bladder outlet obstruction, although the bladder may bear a resemblance to that of a patient with PUV. Similarly, although ureteral dilation in otherwise normal infants is commonly associated with vesicoureteral reflux or obstruction, a similar ureteral lesion in a patient with prune-belly syndrome may occur in the absence of reflux or obstruction. 115.What other anomalies occur outside the genitourinary system in infants with prune-belly syndrome? What are their causes?Patients with prune-belly syndrome often have additional problems, including pulmonary hypoplasia and Potter facies (flattening of the nose, redundant skin, receding chin, ocular hypertelorism, and low-set ears); hip dislocation or subluxation; talipes equinovarus; congenital cardiac disease, especially atrial septal defect, ventricular septal defect, and tetralogy of Fallot; and gastrointestinal anomalies. The urologic/renal dysfunction in patients with prune-belly syndrome is almost certainly responsible for some of the nonurologic complications.
For example, oligohydramnios, a common complication of prune-belly syndrome pregnancies, accounts for the pulmonary hypoplasia, the hip dislocation or subluxation, and the talipes equinovarus that may be seen in these newborns. It has been suggested that the underlying defect in prune-belly syndrome is abnormal mesoderm development.
116.Which diagnostic studies assist the neonatologist in evaluating a child with prune-belly syndrome?The initial work-up should include (1) abdominal and pelvic ultrasonography to provide a basic road map of the genitourinary anomalies and (2) voiding cystourethrography to diagnose vesicoureteral reflux and reflux into a patent urachus. Either of these two diagnoses mandates initiation of antibiotic prophylaxis.
If the infant is stable enough to be transported, other imaging studies significantly enhance understanding of the genitourinary pathology. Computerized axial tomograms of the abdomen, performed before and after intravenous administration of radiocontrast material, will usually reveal more anatomic detail than ultrasound; in addition, they provide a qualitative assessment of comparative renal function (i.e., right versus left kidney). A renal scan using DTPA or MAG3 will localize any points of obstruction between the kidneys and the bladder and provides a quantitative estimate of the comparative function of the two kidneys.
Because an infant with prune-belly syndrome may also harbor gastrointestinal and cardiac anomalies, an upper gastrointestinal tract series with small bowel follow-through, a barium enema, an electrocardiogram, and an echocardiogram are also needed as part of the initial work-up. 117.What is the role for surgical intervention in patients with prune-belly syndrome?Every newborn with prune-belly syndrome should be evaluated by a pediatric urologist. However, intervention during the newborn period should be limited to the least invasive procedures available and should be used only when necessary to relieve high-grade obstruction in the urinary tract. More extensive genitourinary reconstructive procedures should be postponed to a later date and, in fact, may not be necessary at all.
There is considerable controversy about whether surgical intervention is appropriate in boys with prune-belly syndrome when their genitourinary anomalies are not associated with obstruction or vesicoureteral reflux.At some point the surgeon must deal with the intraabdominal cryptorchidism. Orchidectomy, as a means to prevent testicular neoplasia, is an option because the reproductive potential of boys with prune-belly syndrome is probably low. An alternate approach is to relocate the abdominal testes into the scrotum by one of a variety of complex surgeries. In any case these surgical interventions can wait until the infant is several months old.Surgical plication of the lax abdominal musculature is important for the psychological well-being of patients with prune-belly syndrome, but this cosmetic reconstruction should probably not be performed in a newborn. Guay-Woodford, in, 2012 Triad Syndrome (Prune-Belly Syndrome, Eagle-Barrett Syndrome)Triad syndrome, also referred to as prune-belly syndrome or Eagle-Barrett syndrome, involves a constellation of anomalies including congenital absence or deficiency of the abdominal wall musculature, gross ureteral dilation, bladder wall thickening, prostatic hypoplasia, and bilateral undescended testes (cryptorchidism). The full syndrome is expressed only in males, and surviving individuals are typically infertile.
Patients with an incomplete syndrome can have anomalies of the abdominal wall musculature, bladder, and upper urinary tract; 3% of these patients are females. Although the specific molecular events have yet to be defined, defects in mesenchymal development appear to cause poor prostate and bladder differentiation, ureteral smooth muscle aplasia with consequent ureteral aperistalsis, and varying degrees of renal dysplasia.
Three fourths of patients with triad syndrome have associated malformations in the cardiopulmonary system, gastrointestinal tract, and skeleton. In the immediate postnatal period, prognosis depends on the severity of extragenitourinary anomalies. Long-term outcome is based on the degree of renal dysplasia and the success of urodynamic management.
Mann, in, 2011 Prune belly syndromePrune belly syndrome (Eagle–Barrett syndrome) is characterised by the association of a lax and markedly thin anterior abdominal wall – ‘prune belly’, prostatic hypoplasia with a dilated and elongated prostatic urethra, grossly distended smooth and thick-walled urinary bladder, bilateral cryptorchidism, dilated refluxing ureters and renal dysplasia. The degree of upper renal tract involvement is variable. At the most severe end of the spectrum there is effectively urethral atresia resulting in megacystis, bilateral severe ectatic hydroureters and bilateral hydronephrosis with accompanying cystic renal dysplasia.Gastrointestinal, respiratory, cardiovascular and musculoskeletal anomalies are also associated with prune belly syndrome. The exact aetiology is unclear but is probably due to a combination of a primary defect in the anterior abdominal wall and severe bladder outflow obstruction.
Females may also present but only with bladder abnormalities and abdominal wall deficiencies. Javid, in, 2018 Prune Belly SyndromePrune belly syndrome (PBS), also known as Eagle–Barrett syndrome, is a rare condition notable for complete or partial lack of abdominal wall muscle and severe genitourinary abnormalities. A major cause of mortality in newborns with PBS is pulmonary hypoplasia, while comprising a major component of long-term morbidity are urinary tract abnormalities that often result in end-stage renal disease ( Seidel et al., 2015; Arlen et al., 2016).
A variety of reconstruction procedures of the abdominal wall have been described that reportedly improve bladder and GI function as well as improve the appearance ( Hassett et al., 2012). Norman Weinzweig MD, FACS, in, 2010 35 What is “prune belly” syndrome?Prune belly syndrome, also known as triad syndrome or Eagle-Barrett syndrome, consists of a triad of anomalies found almost exclusively in newborn boys: (1) absent or hypoplastic abdominal wall musculature, (2) bilateral cryptorchidism, and (3) dilation of the urinary tract. On physical examination, the muscular deficiency may be limited to one area, ranging from complete absence of muscle to the presence of all muscles as thin but recognizable structures. Complete absence of lower rectus muscles is most common. The abdomen appears as wrinkled or flabby, much like a prune, because of the weakened abdominal wall. As the child grows, the body contour resembles a pear or pot belly more than a prune.
Children are often subject to respiratory complications due to impaired diaphragmatic motion and scoliosis due to the absence of the abdominal support mechanism. Reports describe the use of tensor fascia lata and rectus femoris muscle flaps to strengthen the abdominal wall. Ben O’Neill Donovan. Kropp, in, 2010 Prune-Belly SyndromePrune-belly syndrome (Eagle-Barrett syndrome, triad syndrome) is readily identified on physical examination by the thin, lax, “prune” appearance of the abdomen. The diagnostic criteria of abdominal wall musculature hypoplasia, large hypotonic bladder with dilated tortuous ureters, and bilateral cryptorchidism are specific for prune-belly syndrome. Associated anomalies include severe urethral stenosis or atresia, megalourethra, and imperforate anus. As with PUV, prenatal megacystis, hydronephrosis, and oligohydramnios are suggestive, although one cannot reliably differentiate in utero between the two.
Initial management includes prophylactic antibiotics, serial serum electrolytes, and a renal ultrasound scan to assess renal parenchyma and extent of dilation. Infection rather than obstruction represents the greatest threat to renal parenchyma. Immediate VCUG can be avoided to limit any urethral instrumentation. If the diagnosis is in question, or if catheterization is performed for any reason, a VCUG can then be performed. A characteristic finding is a large-capacity bladder, often with an elongated hourglass appearance of a wide urachal diverticulum (or pseudodiverticulum); 85% have VUR. A dilated proximal urethra is often seen, which can be difficult to distinguish from PUV.
In prune-belly syndrome, prostatic hypoplasia is responsible for the urethral dilation, and a wide bladder neck is seen instead of the bladder neck hypertrophy that is seen in PUV ( Fig. Although the exact pathophysiology behind the urologic manifestations is not well understood, it is generally believed not to be a true outlet obstruction. Rarely does an infant with prune-belly syndrome need emergent intervention. The immediate problems are usually pulmonary (pneumothorax and pneumomediastinum are common). Renal failure may be evident, however. Any instrumentation of the urethra exposes the child to infections that can be difficult to eradicate; a conservative approach is the best initial choice.
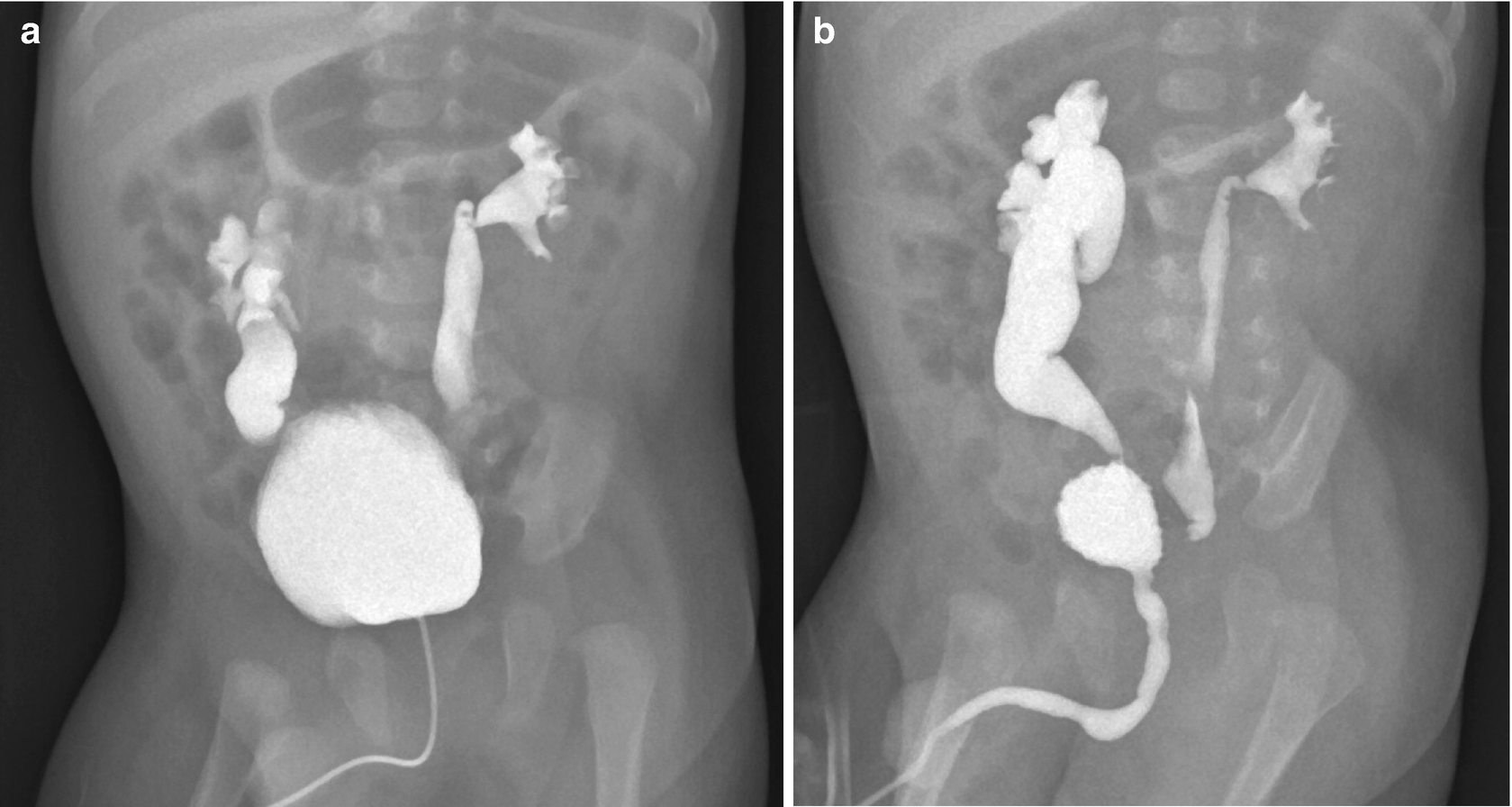
Figure 54-10. Comparison of posterior urethra in prune-belly syndrome and posterior urethral valve. A, Left anterior oblique view of the bladder in a patient with prune-belly syndrome shows the dilated bladder and posterior urethra mimicking a posterior urethral valve. Note the bladder is elongated and at the dome (not shown) gives a false impression of urachal cyst or remnant often giving an hourglass appearance.
Dilation of the posterior urethra is also seen, and this is due to hypoplasia of the prostate and the lack of thickening of the base of the bladder. This distinctly differs from the appearance of the posterior urethra in a patient with posterior urethral valve ( B). B, Left anterior oblique view of bladder in a patient with posterior urethral valve shows the thickened bladder neck and dilated posterior urethra; the posterior urethral valve also is seen. Note the distinction in the appearance from A.Although approximately 50% void spontaneously, the true bladder function requires an ongoing evaluation. In the setting of deteriorating bladder function or persistent infection, a cutaneous vesicostomy should be considered with plans for future undiversion tailored for the individual patient.
The classic wrinkled abdominal wall seen in prune-belly syndrome is accompanied by bilateral undescended testes (A). Affected patients will have marked hydronephrosis.
In severe cases as illustrated here, these small kidneys may have a markedly dysmorphic sonographic appearance (B), and renal insufficiency may be present from the beginning. In cases with severe renal insufficiency, pulmonary development may be compromised, as evident on the radiograph (C); the patient required prolonged mechanical ventilation in the neonatal period.Prognosis ranges from death in utero to near normal life expectancy. Management of the disorder depends on the severity of the symptoms. Patients with incomplete bladder emptying and recurrent UTIs may require a vesicostomy. All male children will have to undergo bilateral orchiopexy before the age of 1 year. Some children will require urinary tract reconstruction and reconstruction of the abdominal wall ( Wheatley et al., 1996).

